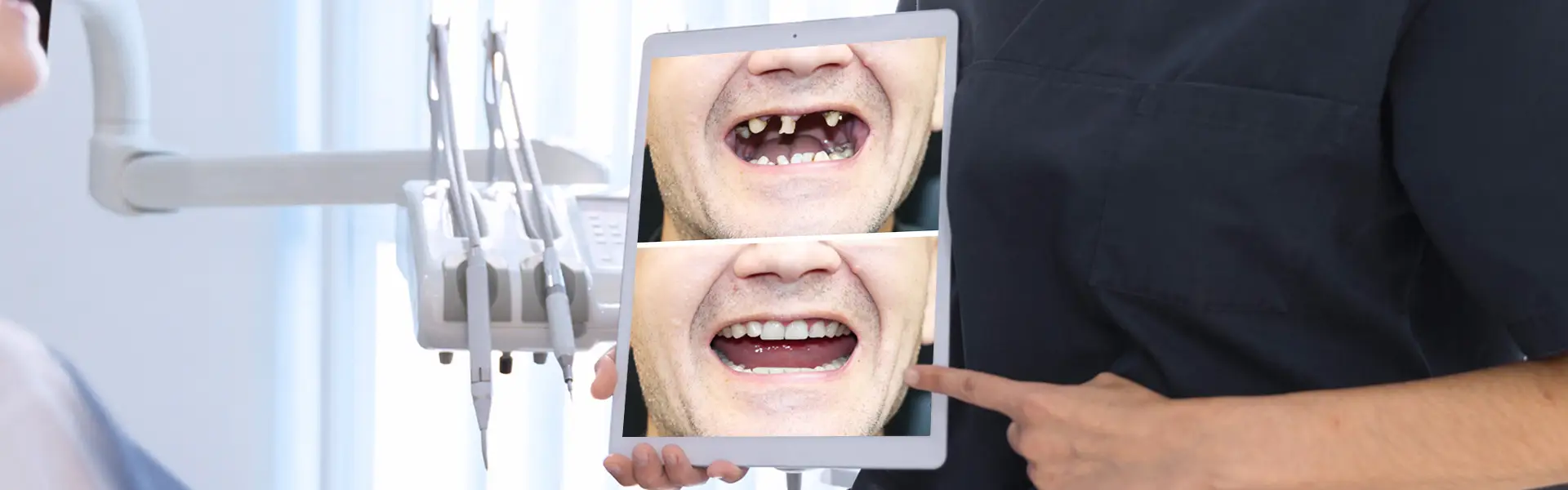
What Procedures Are Included in Full-Mouth Reconstruction?
Extensive dental breakdown can affect multiple teeth, the supporting bone, and gum attachment at the same time. During consultation, radiographs are reviewed to measure remaining bone height and detect infection near root tips. Each tooth is tested for nerve response to determine whether pulp tissue is inflamed or nonvital. Bite alignment is also analyzed to understand how chewing force distributes across both arches. When findings show that isolated restorations would not stabilize the overall structure, Full mouth reconstruction in Waco TX may be discussed as a comprehensive option to protect bone support and restore functional balance.
What Full-Mouth Reconstruction Is Designed to Address
Loss of enamel from grinding or erosion alters how pressure travels into dentin and jawbone. Concentrated force can inflame the periodontal ligament and gradually reduce attachment levels. A restorative dentist in Waco TX measures pocket depth, evaluates bleeding response, and examines joint movement before outlining options.
Repeated fractures, shifting teeth, or mobility often indicate that occlusion no longer distributes load evenly. Collapse of posterior support may increase joint strain and muscle fatigue. Treatment becomes appropriate when structural imbalance risks further bone loss or when remaining tooth structure cannot tolerate functional stress. Decisions depend on bone quality, degree of inflammation, and long-term stability.
Common Dental Issues That Lead to Full Reconstruction
Untreated decay permits bacteria to penetrate enamel and infect pulp tissue. Once infection progresses beyond the apex, surrounding bone may begin to resorb. Periodontal disease weakens connective fibers and reduces tooth stability within the socket.
Chronic grinding shortens crown height and decreases vertical dimension, altering alignment. Vertical root fractures extending beneath the gumline frequently compromise bone support and limit restorative options. When these conditions affect several teeth, rebuilding the entire occlusal system may reduce ongoing breakdown more effectively than addressing teeth individually. Clinical judgment relies on bone levels, mobility, and evidence of active infection.
Procedures Typically Involved in a Treatment Plan
After imaging and bite analysis, treatment is arranged in stages based on infection control and healing capacity.
- Periodontal therapy: Bacterial deposits are removed from beneath the gumline to reduce inflammation and allow tissue reattachment. Healing response is reassessed before proceeding.
- Extractions: Teeth with severe bone loss or vertical fracture are removed to eliminate infection and protect adjacent structures.
- Bone grafting: Graft material is placed when ridge dimensions are insufficient for implant stability. Regeneration is evaluated over several months.
- Dental implants: Titanium fixtures are positioned within the jawbone to permit integration with surrounding bone cells. Stability is confirmed prior to restoration.
- Crowns and bridges: Teeth are reshaped to support restorations that redistribute biting forces across aligned surfaces.
- Root canal therapy: Infected pulp tissue is removed, canals are disinfected, and the space is sealed to reduce risk of reinfection.
A dentist in Waco TX sequences these steps according to clot formation, bone integration, and soft tissue response rather than convenience.
How Reconstruction Restores Function and Comfort
Correcting occlusion reduces excessive pressure on isolated teeth and limits strain on temporomandibular joints. Contact points are adjusted so force spreads more evenly during chewing. Balanced alignment helps protect supporting bone from overload.
Implants transfer functional load into the jawbone in a way similar to natural roots. Successful integration supports maintenance of bone density, provided inflammation does not develop around the implant collar. Gum tissue surrounding crowns and bridges is examined at follow-up visits because marginal irritation can compromise attachment. Ongoing evaluation helps detect early changes before significant breakdown occurs.
Treatment Planning and Sequencing Explained
Comprehensive planning includes radiographs and, when indicated, three-dimensional imaging to measure bone thickness and identify anatomical limitations. Diagnostic models assist in evaluating spacing and occlusal relationships.
Treatment commonly progresses through structured phases:
- Disease Control Phase: Active infection is treated, and non-restorable teeth are removed to stabilize surrounding tissue.
- Foundation Phase: Bone grafting or implant placement is performed if bone volume allows predictable healing.
- Restorative Phase: Definitive crowns or bridges are placed once bone integration and soft tissue health are confirmed.
- Occlusal Adjustment Phase: Bite contacts are refined to reduce uneven loading.
Patients searching for a dentist near me often ask about treatment length. Duration depends on bone density, immune response, and absence of postoperative complications rather than a predetermined timeline.
Recovery and Long-Term Care Considerations
Healing after surgical procedures depends on clot stability and immune function. A stable blood clot protects exposed bone following extraction. Premature disruption may delay tissue repair and increase discomfort. Swelling reflects the body’s inflammatory response and is reviewed during follow-up examinations.
Implants are checked for mobility during the integration period. If sufficient fusion between bone and implant does not occur, further intervention may be required. Margins around crowns and bridges are inspected to reduce bacterial infiltration. Long-term stability relies on preserving gum attachment and observing bone levels at periodic intervals.
Supporting Oral Health After Reconstruction
Consistent plaque control reduces bacterial accumulation that can inflame gingival tissue and weaken bone support. Gentle brushing protects the gum margin while minimizing recession. Interdental cleaning prevents debris from collecting around implant components and restoration edges.
Nightguards may be recommended if grinding places excessive force on reconstructed teeth. Periodic examinations and radiographs allow early detection of bone changes or tissue irritation. Reconstructed teeth and implants remain biologically integrated with surrounding structures and respond to stress over time.
Final Thoughts
Full-mouth reconstruction requires elimination of infection, correction of occlusal imbalance, and preservation of existing bone before definitive restorations are placed. Each decision is guided by structural findings and healing response rather than cosmetic preference. At Hillcrest Dental Care, reconstruction planning follows careful evaluation of bone condition, tissue attachment, and functional alignment, with scheduled reassessment to reduce the likelihood of future complications.
